The word ‘eczema’ is originally Greek, meaning ‘to boil’. In the original description of eczema, ‘bubbles’ under the skin, was the main finding. Today, it is defined as a group of inflammatory skin conditions. With gathering research and experience, at least five types of eczema are defined (atopic, discoid, irritant, allergic and asteototic).
 Eczema affects both men and women equally, usually appearing in the first weeks or months of an individual’s life. It is most common in children, affecting at least 10% of infants at some stage. For many, eczema will disappear during childhood, although it can continue into adulthood or reappear in teenage or early adult years. Not infrequently, eczema can appear for the first time in adulthood.
Eczema affects both men and women equally, usually appearing in the first weeks or months of an individual’s life. It is most common in children, affecting at least 10% of infants at some stage. For many, eczema will disappear during childhood, although it can continue into adulthood or reappear in teenage or early adult years. Not infrequently, eczema can appear for the first time in adulthood.
One of the most common questions asked of a dermatologist is ‘what am I reacting to?’ or ‘is it something in my diet?’
The majority of eczema (about 80%) is ‘internal’, meaning not related to any outside cause. This same group of people, however, have a higher tendency to allergies. To add another complication, these allergies are often not related to the eczema itself! For instance, many eczema sufferers have an allergy to pollen, but pollen does not affect their eczema.
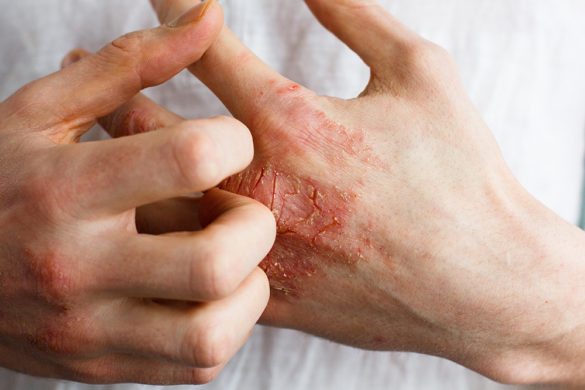
Although it is not fully understood, eczema often runs in families, and is part of genetic makeup. It can affect any part of the skin, including the face, but the area’s most commonly affected are the bends of the elbows and knees and around the wrists and neck. It mostly occurs as red and dry skin which cause uncomfortable itching.
With Winter upon us, the cold, dry air can cause eczema to worsen for many. With many of us going from icy temperatures to blasts of dry central heating throughout the day, the lack of humidity in the air can cause skin to become dry, making it difficult to maintain moisture.
It isn’t just the temperatures that cause eczema flare-ups, but also certain types of clothing. By wearing wool, or rough fabrics, they can chafe and irritate the skin causing the condition to worsen.
In modern medicine, there is a multitude of eczema treatments which can be prescribed by a dermatologist, and excellent control can be gained with the right management. Your treatment will be dependent on your medical background, severity and extent of condition and other personal factors.
The biggest message is, don’t spend years hunting for an allergy (for adults or children). There often isn’t a relevant one found, and a dermatologist can help navigate when it’s worth investigating further.
What can I do?
- Avoid excessive use of known irritants; perfumed soaps, bubble baths, biological washing powders and fabric conditions. During a flare, limit their use as far as possible and reduce your bath or shower times until your skin improves.
- Look out for signs of infection. Infected eczema often gets progressively worse with your ‘normal’ treatments and requires temporary alteration and possible inclusion of antibiotics to your regime.
- Moisturise the skin ‘as often as appropriate’. You may only need to moisturise the torso and arms once a day, but your hands may need moisturising 4 to five times a day. This varies between individuals depending on their specific pattern.


